Let’s face it: there are many types of migraine [1]. This is complicated even for physicians, especially family docs who do not receive a lot of training on migraine during their residency. It is important to understand those terms as specific characteristics might influence your investigations and treatments.
Here is a guide to help you define your situation.
See our LINKS to learn more about each type!
Who decided how to diagnose migraine?
Health care providers and researchers use the International Headache Disorders Classification. This is available online [2]. The criteria are determined by experts and researchers based on experience and studies on big groups:
How is migraine diagnosed?
There is currently NO blood work or imaging test that can prove that you have migraine. (See this post [3]). The diagnosis is based on symptoms and making sure that there is no other cause for the headache (the famous SNOOPPPP red flags [4]).
Typical symptoms used to diagnose migraine are:
- Recurrent attacks: remember that if you have a new type of headache, it could be something else than migraine and you should seek medical advice.
- Duration of attacks: 4 hours to 3 days
- Type of headache: typically one-sided, moderate to severe, and throbbing, but not everyone fits those criteria.
- Other symptoms: there is a big focus on nausea, light and sound sensitivity, but other symptoms like smell sensitivity, neck pain, difficulty to focus and dizziness [5] are often part of the attack.
Once you have received diagnosis of migraine, it’s not enough. You have to define the situation more precisely to choose the right treatment. Let’s look at categories.
Migraine categorized by frequency:
- Episodic migraine: when you have less then 15 days per month of migraine/headaches.
- Frequent episodic: a category still in definition, it described people who are not chronic but have migraine «often», like 7 to 14 days per month.
- Chronic migraine [6]: the most severe form of migraine, if you have 15 days or more of headache per month, including 8 days with migraine symptoms.
Remember that migraine frequency fluctuates, and we know now that many patients may have a very bad month in the «chronic» category, then go back down to episodic. We call this the roller coaster of migraine.
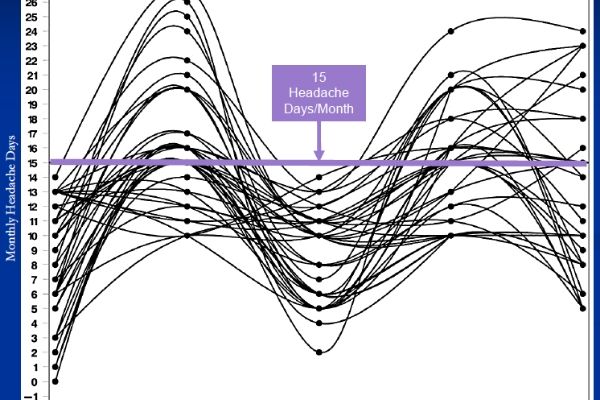
For this reason, some researchers now believe that putting people with migraine in boxes does not represent the true continuum of migraine. It may be important for research to create categories, but the real life is more complicated.
Migraine categorized by symptoms:
Migraine with aura [7]:
The official classification puts a lot of importance on this particular symptom, as we understand quite a lot about the aura [8] and in migraine history this subgroup of patients has been well studied. (See this post [9])
- Typical visual aura: any visual symptom with typical characteristics.
- Complex aura: problems with speech and sensation (numbness or tingling). This will often make your physician nervous and justify a workup.
- Hemiplegic migraine [10]: presence of auras with true weakness of a limb AND also other typical auras. There should always be a full workup and ideally genetic testing. (See this post [11])
What if I have auras, but no headache?
It is not uncommon to see a 40-50-60 years old person having a very typical migraine aura with NO headache and no history of migraine. This should remind us that the aura and the migraine have different brain mechanisms and that the aura may occur without any headache.
Vestibular migraine:
This is the very disagreeable combination of migraine and dizziness and vertigo (vestibular symptoms). This is still a controversial entity, and a lot of research is ongoing. (See this post [12])
Migraine categorized by triggers:
The Classification does not endorse many official categories by triggers, even if these are frequently used by the public. For example, «sinus migraines», «weather migraines» and «neck migraines» make sense to people but are not official categories.
Migraine researchers tend to see migraine as a disorder of the brain (See this post [13]) and argue that if we start diagnosing by triggers, we’ll end up with too many categories. There is one exception to this rule, which is menstrual migraine [14].
Menstrual migraine: if migraine occurs reliably over the -2 to +3 days of bleeding, then this could be your diagnosis. Remember that if you have frequent or chronic migraine, overlap with the period might be random and that you should start with overall migraine control before using specific menstrual migraine techniques.
Chronic migraine categorized with or without medication overuse
The topic of medication overuse is a difficult one (See this post [15]). Sadly, people with migraine tend to worsen if they use acute treatments frequently (even with no addiction). Limit numbers of days with medication use come from big database research.
Overall, the official cutoffs for overuse are:
- 10 days/month for: opioid, triptans [16], any combination of medications
- 15 days/month for acetaminophen OR NSAIDs ONLY.
Refractory migraine: a category based on treatment response and severity
There is no official agreement for its definition. Refractory means that treatments do not work. We often link it with chronic migraine, but episodic migraine could also be refractory. Usually, 2 to 4 recognized preventive treatments have to be ineffective to use this term. In general, refractory migraine is also severe and disabling.
Migraine equivalents of childhood
Symptoms that occur mostly in children, may not be accompanied by headaches, and are thought to be linked with future migraine (See this post [17]). These include
- Abdominal migraine [18]
- Cyclical vomiting syndrome
- Paroxysmal vertigo
- Paroxysmal torticollis
- Colics
In summary, a migraine diagnosis is not enough.
You and your health care provider should have a good global overview of your personal picture. A headache diary like the Canadian Migraine Tracker App [19] may be very helpful to clarify the situation. A clear view will guide your treatment decisions!
Post#101
