Migraine attacks can be triggered by various factors. While it’s impossible to avoid all triggers, identifying your specific ones through a migraine diary can be helpful. Understanding the difference between premonitory symptoms and actual triggers is crucial for effective management. Maintaining a consistent routine with regular sleep, meals, and exercise can raise your migraine threshold and help you better cope with triggers. Explore strategies for balancing trigger management and overall migraine prevention in this comprehensive guide.
What are migraine triggers?
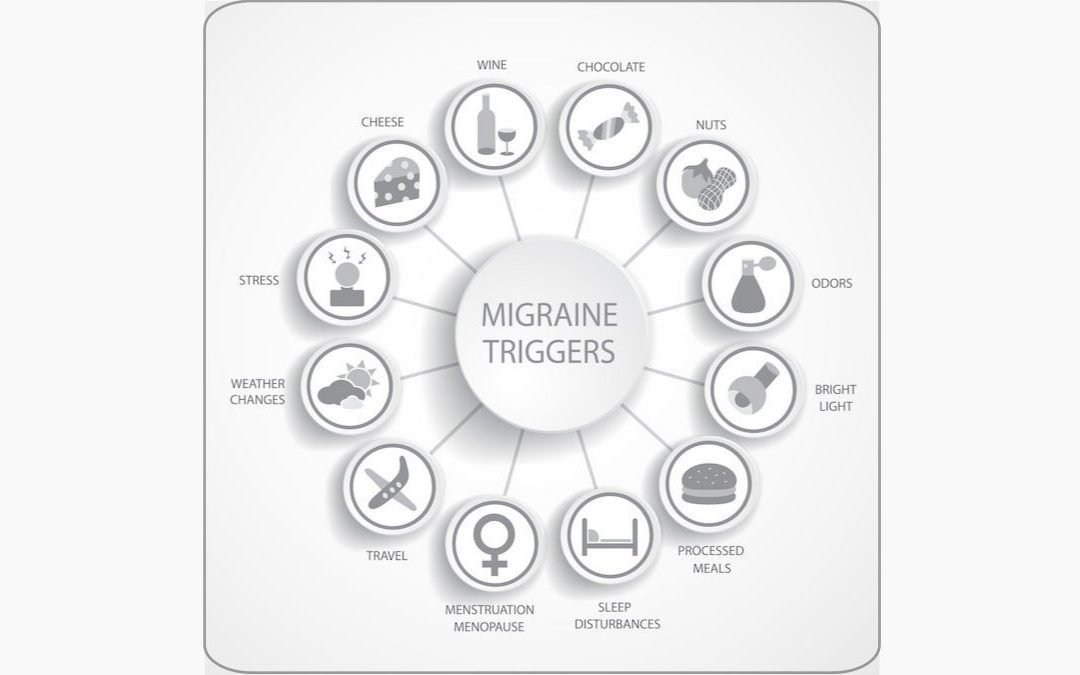
Migraine triggers are factors that can initiate a migraine attack. These triggers can be internal, like hormones and emotions, or external, like weather changes and smells. Sometimes, internal and external triggers interact, such as drinking alcohol to relieve anxiety. Some triggers are within your control, while others are not.
Which things can trigger a migraine?
Many researchers have surveyed patients about their perceived triggers. The list of potential migraine triggers is very long:
Should I avoid all triggers?
Avoiding all triggers is unrealistic. Triggers are unique to each individual, and you likely won’t be affected by every potential trigger. Identifying your specific triggers can take time and effort.
Identifying Your Triggers
Keeping a migraine diary is an effective way to identify patterns over time. Apps like the Canadian Migraine Tracker, Migraine Buddy, and Curelator can assist in tracking triggers and healthy practices. If migraine attacks are frequent, it is more difficult to identify single triggers. It may be better to stop the trigger chase to focus on protective behaviours and medications.

Premonitory Symptoms vs. Triggers
The premonitory phase of a migraine occurs before the pain starts, with symptoms like fatigue, stress, or appetite loss. It can be challenging to distinguish whether a symptom is a premonitory sign or a trigger. An example is: Did skipping a meal trigger your migraine, or were you in the first phase of a migraine and didn’t have an appetite?
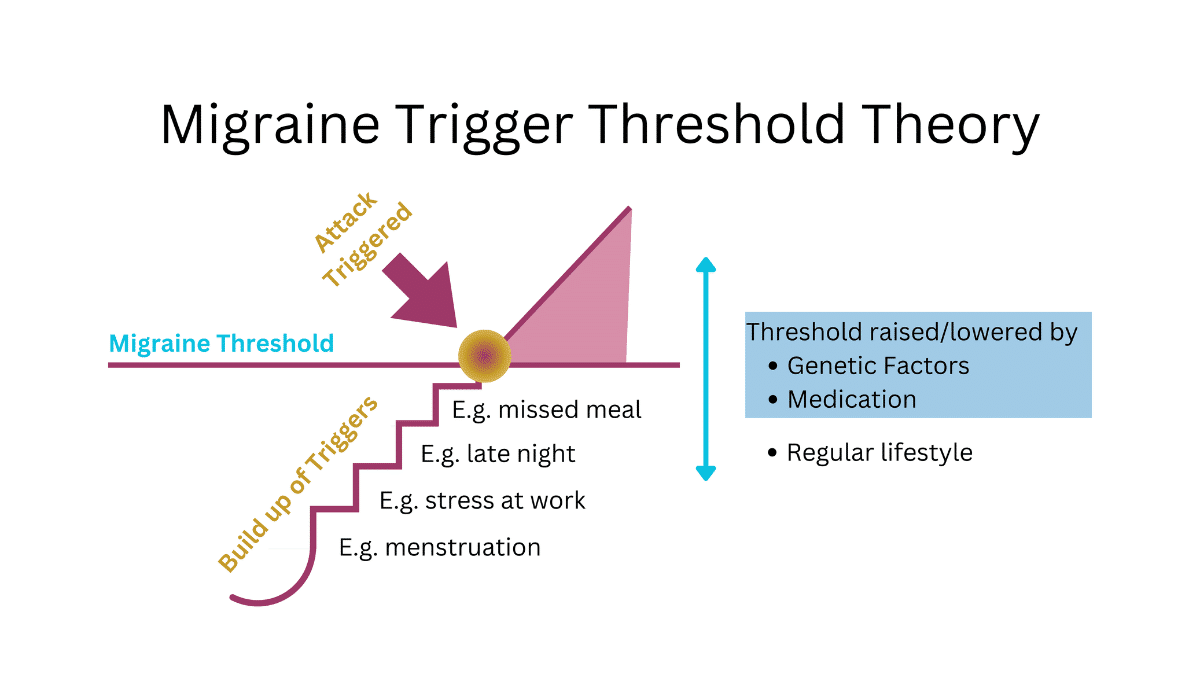
Migraine Trigger Threshold Theory
Triggers can accumulate, meaning a single trigger might not cause an attack, but a combination might. For example, you might not get a migraine from stress alone, but stress combined with lack of sleep and alcohol could trigger an attack.
Building Resistance to Triggers
There is a theory that gradual exposure to small amounts of a trigger may build tolerance, but this research is ongoing. This might apply to triggers like foods or stress but is impractical for others like weather changes.
Raising Your Migraine Threshold
Maintaining consistency in your daily routine can help raise your migraine threshold. Regular sleep, meals, hydration, exercise, relaxation, and preventive medications can raise your threshold so that more triggers can stack up before an attack occurs.
The Importance of Managing Triggers
While managing triggers is helpful, it’s essential to avoid becoming overly rigid, as this can add stress. A balanced approach, possibly including medication, is crucial for effective migraine management.
References
- Spierings EL, Donoghue S, Mian A, Wober C. Sufficiency and necessity in migraine: how do we figure out if triggers are absolute or partial and, if partial, additive or potentiating? Curr Pain Headache Rep. 2014;18(10):455.
- Baldacci F, Vedovello M, Ulivi M, Vergallo A, Poletti M, Borelli P, et al. How aware are migraineurs of their triggers? Headache. 2013;53(5):834-7.
- Andress-Rothrock D, King W, Rothrock J. An analysis of migraine triggers in a clinic-based population. Headache. 2010;50(8):1366-70.
Post #009